Skin Atrophy and Infections from Topical Corticosteroids: Causes, Risks, and Recovery
 May, 7 2026
May, 7 2026
Topical Steroid Risk & Recovery Estimator
Assessment Parameters
Low Risk
Based on current inputs, the risk of significant skin atrophy is minimal. Monitor for any changes in skin texture.
N/A
That tube of cream sitting in your bathroom cabinet is likely a topical corticosteroid, which is a potent anti-inflammatory medication used to treat conditions like eczema, psoriasis, and dermatitis. It works wonders for stopping the itch and redness. But there is a hidden cost that many users don’t see until it’s too late. Long-term or improper use can lead to skin atrophy, defined as the thinning and weakening of the skin layers due to suppressed cell production, and an increased susceptibility to stubborn skin infections, caused by bacterial, fungal, or viral overgrowth resulting from localized immune suppression.
You might think these side effects only happen if you misuse the drug. The truth is more concerning. Even short-term application of high-potency steroids can alter the structure of your epidermis. Understanding how this damage happens, recognizing the early signs, and knowing how to repair your skin barrier is crucial for anyone relying on these medications.
How Steroids Thinning Your Skin Works
To understand why your skin gets thin, you have to look at what happens under the surface. Your skin relies on two main types of cells to stay thick and resilient: keratinocytes, which are the primary cells in the epidermis responsible for producing structural proteins, and fibroblasts, which are cells in the dermis that produce collagen and elastin.
When you apply a corticosteroid, it binds to receptors in these cells. This triggers a chain reaction that slows down cell division. Specifically, it reduces the synthesis of extracellular matrix (ECM), which is the network of proteins and carbohydrates that provides structural support to tissues. Without enough ECM, your skin loses its tensile strength and elasticity.
The most significant change involves collagen, which is the primary protein responsible for skin firmness and thickness. Steroids inhibit the genes that code for type I and type III collagen. They do this by interfering with Smad proteins, which are necessary for collagen transcription. Research published in Frontiers in Allergy (2025) shows that this inhibition happens quickly. Even after just three days of using potent glucocorticoids, you can see changes in epidermal structure. While the visible signs might not appear immediately, the stratum corneum, which is the outermost layer of the skin that acts as a protective barrier, begins to recover slowly, often lagging behind the rest of the tissue.
This process creates what doctors call "elephant wrinkles"-deep folds that resemble elephant skin. These aren't just cosmetic issues; they signal a breakdown in the skin's ability to protect itself from the environment.
The Hidden Risk of Skin Infections
Thinning skin is dangerous enough, but it opens the door to another problem: infections. Topical corticosteroids are immunosuppressants. They calm inflammation by dampening your local immune response. This is great for stopping an allergic reaction, but it also means your skin can’t fight off invaders as effectively.
Here is how the cycle typically plays out:
- Bacterial Overgrowth: With reduced immune surveillance, bacteria like Staphylococcus aureus can multiply rapidly on compromised skin. This often leads to impetigo or cellulitis.
- Fungal Flares: Fungi thrive in warm, moist environments. If you are using steroids on intertriginous areas (skin folds), you create a perfect breeding ground for yeast and ringworm. Interestingly, steroids can mask the typical redness of a fungal infection, making it harder to diagnose-a condition known as tinea incognito, which is a fungal infection that has been altered by steroid use, often appearing less red but more widespread.
- Viral Reactivation: Herpes simplex virus (cold sores) or molluscum contagiosum can spread more easily when the skin barrier is weakened and the immune response is suppressed.
A study in American Family Physician (2021) highlighted that acneiform eruptions occur in about 3.1% of long-term users. This isn't regular acne; it's a sterile pustule formation driven by the alteration of skin flora and follicular plugging caused by the medication.
Who Is Most at Risk?
Not everyone who uses topical steroids will develop severe atrophy. However, certain factors significantly increase your risk profile. Understanding where you fall on this spectrum helps you make safer choices.
| Risk Factor | Why It Increases Risk | Clinical Impact |
|---|---|---|
| Skin Thickness | Thin skin absorbs more medication systemically and has less reserve tissue. | Face, eyelids, groin, and armpits are 3-5 times more susceptible than arms or legs. |
| Potency Class | Higher potency classes (I-IV) suppress collagen synthesis more aggressively. | Class I steroids carry a substantially higher risk of permanent striae compared to Class VII. |
| Duration of Use | Long-term use prevents natural cell turnover and repair mechanisms. | Atrophy occurs in approximately 17% of long-term users according to meta-analyses. |
| Age | Children and elderly individuals have thinner skin and slower regeneration rates. | Children are particularly vulnerable to growth suppression and permanent scarring. |
| Occlusion | Covering treated skin with bandages or plastic increases absorption up to 100x. | Significantly accelerates atrophy and systemic side effects. |
If you are applying a high-potency steroid to your face for more than two weeks, you are playing a high-stakes game. The American Academy of Dermatology strongly advises against this practice. Thin skin areas simply cannot handle the same dosage as thicker skin on your back or palms.
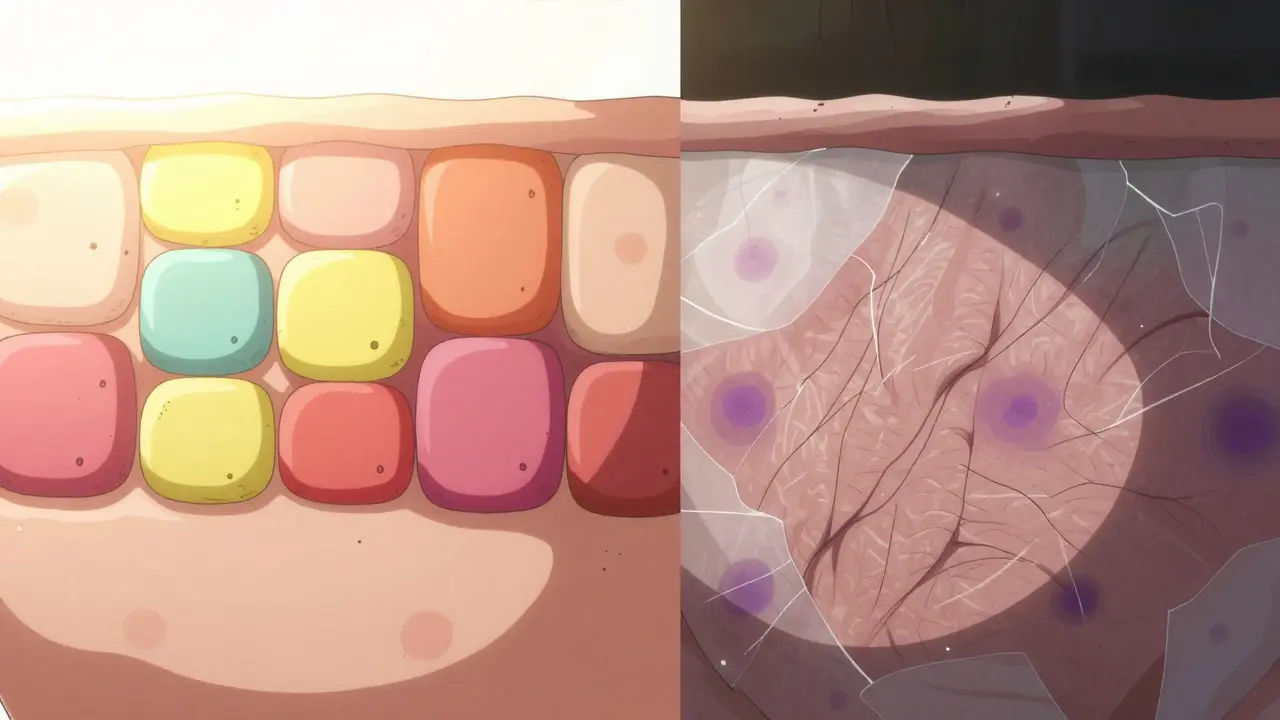
Recognizing the Signs Early
Catching atrophy early can prevent permanent damage. What should you look for? It’s not always obvious because the skin might still look smooth initially. Here are the subtle clues:
- Translucency: You can see blood vessels clearly through the skin. This is called telangiectasia. The skin looks shiny and waxy.
- Purpura: Small purple spots appear after minor bumps or scratches. This happens because the capillaries lose their surrounding support structure and rupture easily.
- Striae: Stretch marks that don’t fade. Unlike normal stretch marks, steroid-induced striae are often wider and more persistent. Once these form, the damage is usually irreversible.
- Perioral Dermatitis: A rash around the mouth that looks like small pimples. This is a classic sign of steroid misuse on the face.
If you notice any of these signs, stop using the product immediately. Do not try to "power through" the irritation. Continuing to apply steroids to already atrophic skin will only worsen the condition and increase the risk of secondary infection.
Navigating Steroid Withdrawal
Stopping cold turkey can be terrifying. Many patients experience Topical Steroid Withdrawal (TSW), which is a severe rebound reaction characterized by intense burning, redness, and peeling after discontinuing steroid use.. This is not just psychological; it’s physiological. Your body has become dependent on the external source of cortisol-like activity to regulate inflammation.
The withdrawal pattern follows a predictable sequence. Mild erythema (redness) appears about one week after cessation. This lasts for two weeks and ends with desquamation (peeling). Then, a second flare occurs within two weeks. Each subsequent flare decreases in duration, but the initial phase can be brutal.
Community data from Reddit forums like r/SteroidAddiction, which hosts over 4,300 active members, suggests that the average recovery time is 8.2 months. Patients report "burning face syndrome," where the pain is disproportionate to the visible redness. This is because nerve endings are exposed due to the thinning of the stratum corneum.
To manage this, gradual tapering is essential. Instead of stopping completely, reduce the frequency of application. For example, go from twice daily to once daily, then every other day. Combine this with non-steroidal alternatives like tacrolimus, which is a calcineurin inhibitor used to treat eczema without causing skin thinning, or pimecrolimus, which is another non-steroidal anti-inflammatory cream suitable for sensitive areas.

Repairing Your Skin Barrier
Once you’ve stopped the steroids, the focus shifts to repair. Your skin barrier is compromised, meaning it loses water faster than normal (increased transepidermal water loss or TEWL). You need to rebuild the lipid matrix.
The gold standard for barrier repair involves specific ratios of lipids. Research indicates that formulations containing ceramides, cholesterol, and free fatty acids in a 3:1:1 molar ratio yield the best results. A 2020 randomized controlled trial showed a 68.4% improvement in skin barrier function after eight weeks of using such formulations.
Look for products labeled "ceramide-rich" or "barrier repair." Avoid harsh cleansers, exfoliants, or active ingredients like retinoids or vitamin C during the initial healing phase. Your skin is too fragile for them right now. Stick to gentle, fragrance-free moisturizers applied immediately after bathing while the skin is still damp.
Sun protection is non-negotiable. UV radiation degrades collagen further. In atrophic regions, unprotected sun exposure increases collagen degradation by 42%. Use a broad-spectrum SPF 50+ sunscreen daily. Physical blockers (zinc oxide or titanium dioxide) are often better tolerated than chemical filters during the TSW phase, as they sit on top of the skin rather than absorbing into it.
Future Alternatives and Safer Options
The medical community is aware of these risks. Regulatory bodies like the FDA and EMA have mandated warnings about atrophogenic potential on packaging. But beyond warnings, new treatments are emerging.
Researchers are developing "dual-soft" glucocorticoid receptor agonists. These molecules aim to maintain anti-inflammatory properties while minimizing the inhibition of collagen synthesis. Additionally, Phase II trials are underway for topical formulations combining low-dose corticosteroids with fibroblast growth factor. Preliminary results show a 63% reduction in atrophy incidence compared to standard treatment.
In the meantime, steroid-sparing therapies are becoming more popular. Non-steroidal options like crisaborole, which is a PDE4 inhibitor approved for mild-to-moderate atopic dermatitis, offer effective relief without the risk of thinning. As awareness grows, the market for these safer alternatives is projected to reach $3.8 billion by 2028.
Can skin atrophy from topical steroids be reversed?
Short-term atrophy can often be reversed by stopping the medication and allowing the skin to heal over several weeks or months. However, permanent damage such as striae (stretch marks) and significant loss of subcutaneous fat is usually irreversible. Early intervention improves the chances of full recovery.
How long does it take for skin to recover after stopping steroids?
Recovery varies widely depending on the potency of the steroid, the duration of use, and the individual's age. Mild cases may resolve in a few weeks. Severe cases involving Topical Steroid Withdrawal (TSW) can take 6 to 12 months or longer for the skin barrier to fully restore and symptoms to subside.
What are the safest alternatives to topical corticosteroids?
Non-steroidal alternatives include calcineurin inhibitors like tacrolimus and pimecrolimus, PDE4 inhibitors like crisaborole, and JAK inhibitors for more severe cases. These medications do not cause skin thinning and are safer for long-term use on sensitive areas like the face and groin.
Why do steroids cause acne?
Steroid-induced acne, or acneiform eruption, occurs because corticosteroids alter the skin's microbiome and cause follicular plugging. It typically presents as small, uniform pustules rather than the varied lesions seen in typical acne vulgaris. It is more common on the face and upper trunk.
Is it safe to use topical steroids on the face?
Only low-potency steroids (Class VI-VII) should be used on the face, and only for short periods (no more than 5-7 days). High-potency steroids should never be used on the face due to the high risk of perioral dermatitis, rosacea-like eruptions, and rapid skin atrophy.
